Many people notice light bleeding while brushing or flossing and assume it is only temporary gum irritation. However, when bleeding happens repeatedly, it may indicate a deeper issue affecting the gums and supporting structures around the teeth. One of the most common long-term gum conditions is periodontitis.
Periodontitis is a progressive form of gum disease that develops gradually over time. Because symptoms often appear slowly, many people do not realize the condition has advanced until noticeable changes occur. Understanding the stages, symptoms, causes, and diagnostic process can help individuals recognize when professional dental evaluation may be necessary.
What Is Periodontitis?
Periodontitis is a chronic inflammatory gum disease that damages the tissues and bone supporting the teeth. It usually begins as mild gum inflammation caused by plaque accumulation near the gum line. Without proper management, the inflammation can spread deeper below the gums and gradually weaken tooth support.
Unlike temporary gum irritation, periodontitis involves structural changes that may progress over months or years. The condition can vary significantly between individuals depending on oral hygiene habits, smoking history, overall health, and genetic factors.
The New Classification System for Periodontitis
Dental professionals now use a modern classification framework that replaced older broad categories of gum disease. This updated system evaluates:
- Stage — how severe the tissue and bone damage is
- Grade — how quickly the disease appears to progress
This approach provides clearer communication between dentists and patients while improving long-term monitoring.
Periodontitis Staging and Grading Explained
Staging focuses on the amount of damage already present, including bone loss and gum attachment loss. Grading evaluates factors that influence disease progression, such as smoking or systemic health conditions.
Together, staging and grading help create a clearer picture of the condition without predicting exact outcomes for every patient.
Also Read: How Smoking Affects Gums? And What You Can Do About It
Common Symptoms of Periodontitis
Symptoms of periodontitis often develop slowly and may initially seem minor. Some people experience only mild discomfort, while others notice more visible gum or tooth changes over time.
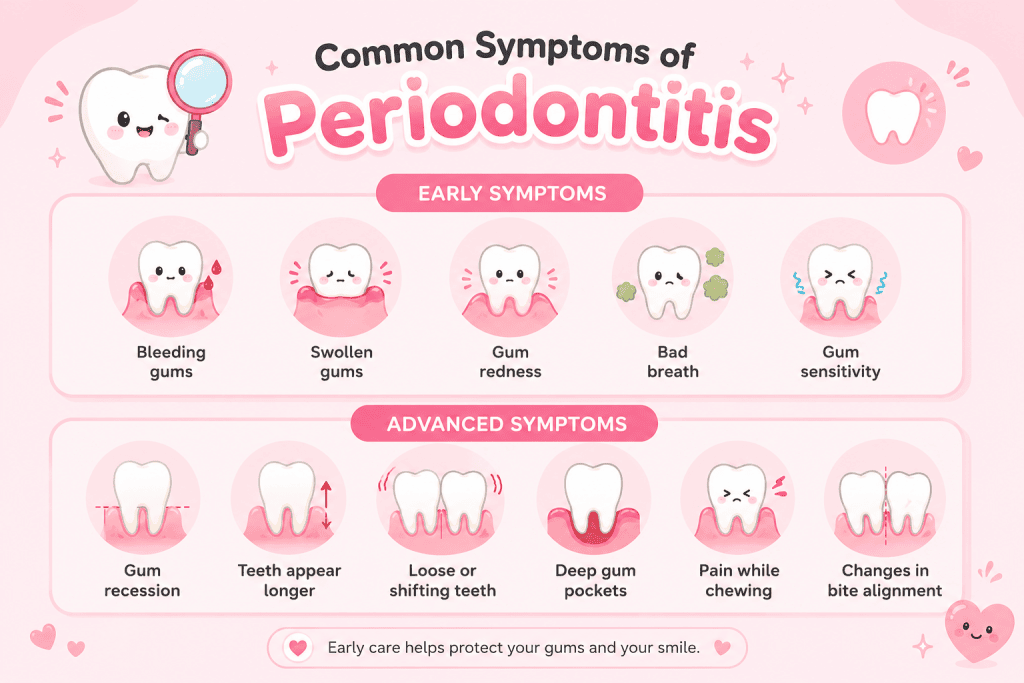
Early Symptoms of Periodontitis
Early warning signs commonly include:
- Bleeding gums during brushing or flossing
- Mild gum swelling
- Gum redness
- Persistent bad breath
- Increased gum sensitivity
These symptoms may come and go, making them easy to ignore at first.
Symptoms of Advanced Periodontitis
As the disease progresses, symptoms may become more noticeable, including:
- Gum recession
- Teeth appearing longer
- Loose or shifting teeth
- Deep gum pockets
- Pain while chewing
- Changes in bite alignment
These changes often suggest longer-term inflammation affecting deeper supporting structures.
| Symptom | Common in Early Disease | More Concerning When Persistent |
|---|---|---|
| Bleeding gums | Occasional during brushing | Regular bleeding even with gentle cleaning |
| Swollen gums | Mild redness or puffiness | Ongoing inflammation |
| Bad breath | Temporary odor | Persistent odor despite hygiene |
| Gum recession | Minimal or absent | Visible root exposure |
| Loose teeth | Not present | Teeth shifting or unstable |
What Causes Periodontitis?
The primary cause of periodontitis is plaque buildup along the gum line. Plaque contains bacteria that trigger the body’s inflammatory response. When plaque is not removed consistently, it hardens into tartar and prolongs gum inflammation.
Over time, this inflammatory process may damage the tissues and bone supporting the teeth.
Plaque and Long-Term Gum Inflammation
Daily plaque accumulation allows bacteria to remain in constant contact with the gums. The body responds by sending inflammatory cells to the area, but long-term inflammation can eventually harm healthy tissue instead of protecting it.
Risk Factors That May Increase Progression
Several factors may increase the risk or speed of progression, including:
- Smoking
- Diabetes or other chronic health conditions
- Family history of gum disease
- Poor oral hygiene
- Chronic stress
- Nutritional deficiencies
These factors do not directly cause periodontitis alone, but they may influence how aggressively the disease develops.
The 4 Stages of Periodontitis
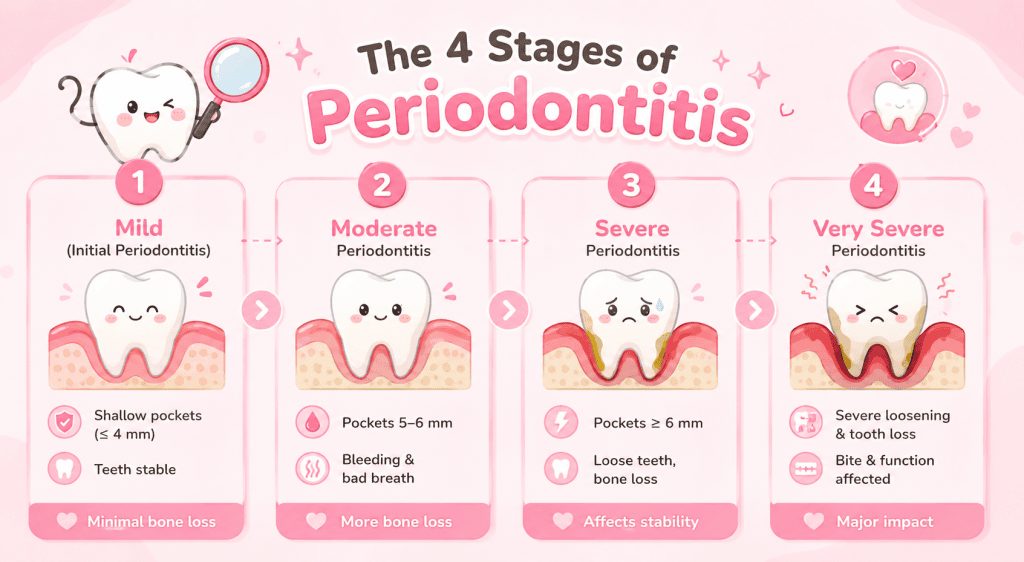
Stage 1 — Mild (Initial Periodontitis)
At this earliest stage, bone loss is minimal and confined to areas just below the gum line. Pockets are shallow (around 4 mm or less) and teeth remain fully stable. Most people notice little to no symptoms, which is why routine dental check-ups are the most reliable way to catch it this early.
Stage 2 — Moderate Periodontitis
Bone loss becomes more noticeable on X-rays, and pockets deepen to around 5–6 mm. Bleeding during brushing happens more regularly, and persistent bad breath may develop. Teeth are still stable at this point, but early gum recession can begin to appear. This stage responds well to professional treatment combined with consistent home care.
Stage 3 — Severe Periodontitis
Pockets reach 6 mm or deeper, and bone loss begins to affect tooth stability. Some teeth may start to feel loose or shift position. Furcation involvement — where bone loss reaches between the roots of multi-rooted teeth — can occur. Sensitivity, discomfort when chewing, and ongoing bad breath are common. Prompt professional evaluation is important at this stage.
Stage 4 — Very Severe Periodontitis
This stage shares the same level of damage as stage 3 but also affects the ability to chew and function normally. Teeth may be severely loose, and some may already be lost. The bite can shift noticeably. Treatment at this point focuses on both halting progression and restoring function, often requiring a more complex and coordinated care plan.
Also Read: Gum Infection: Symptoms, Causes & Treatment
How Periodontitis Is Diagnosed
Diagnosis involves combining several types of clinical findings rather than relying on one single test.
Dental Examination and Gum Measurements
During a periodontal assessment, a dental professional measures the depth between the gums and teeth using a periodontal probe. Other observations may include:
- Bleeding on probing
- Gum recession
- Plaque accumulation
- Tooth mobility
These measurements help determine the stage and severity of disease involvement.
Periodontitis X-Ray Findings
Dental x-rays play an important role in identifying bone loss beneath the gum line.
Early x-ray findings may show mild horizontal bone loss, while more advanced disease can reveal:
- Vertical bone defects
- Furcation involvement
- Reduced bone support around roots
Radiographs also help track changes over time.
| Diagnostic Tool | What It Shows | Why It Matters |
|---|---|---|
| Probing depths | Space between tooth and gum | Measures attachment loss |
| Bleeding on probing | Active inflammation | Identifies irritated areas |
| Bitewing or periapical x-rays | Bone levels | Detects hidden bone loss |
| Full-mouth imaging | Overall support pattern | Helps determine staging |
Why Staging and Grading Matter
Staging and grading convert clinical measurements into a structured description that supports clearer communication, long-term monitoring, and individualized care planning.
Periodontitis Treatment and what people commonly search for
Many people search for whether periodontitis can be reversed or managed at home. Professional evaluation remains the step that determines what approaches are appropriate for each individual case.
Can periodontitis be cured?
The intent behind searches like “how to cure periodontitis” is usually informational: people want to know if progression can be stopped or improved. Exact outcomes depend on the stage at the time of assessment and the consistency of ongoing care.
Periodontitis Toothpaste and Oral Care Products
Searches for gum-focused toothpastes reflect genuine interest in daily habits that support gum health. These products can be part of broader routines but do not replace professional measurement of pocket depths or bone levels.
Periodontitis Oil Pulling and Natural Remedies
Oil pulling appears in searches as a traditional practice some people try. Available information indicates it does not replace mechanical plaque removal or professional assessment — but it can be discussed during a dental visit to understand how it may or may not fit into overall care.
When to See a Dentist
Certain symptoms should not be ignored, especially when they persist for weeks or worsen over time.
Signs That Need Professional Attention
Consider scheduling a dental evaluation if you experience:
- Persistent gum bleeding
- Ongoing bad breath
- Gum recession
- Loose teeth
- Swollen gums that do not improve
Even mild symptoms can help establish an early baseline for monitoring.
When Urgent Assessment May Be Necessary
Immediate dental attention may be needed if symptoms include:
- Sudden swelling
- Severe pain
- Gum discharge or pus
- Rapid tooth mobility
These signs may indicate active infection requiring prompt evaluation.
Preventing Periodontitis and Slowing Progression
Although periodontitis cannot always be fully prevented, consistent oral care and regular monitoring may reduce risk and slow disease progression.
Daily Oral Hygiene and Professional Cleaning
Healthy oral habits typically include:
- Brushing twice daily
- Daily flossing
- Regular professional cleanings
- Routine dental examinations
Professional cleanings remove hardened tartar that cannot be eliminated through brushing alone.
Lifestyle Habits That Support Gum Health
Several habits may support healthier gums, including:
- Avoiding smoking
- Managing blood sugar levels
- Eating a balanced diet
- Reducing chronic stress
These factors work alongside professional dental care rather than replacing it.
Can Periodontitis Affect Overall Health?
Some people search whether periodontitis can become life-threatening. While periodontitis itself is not generally described in those terms, long-term gum inflammation has been associated with broader systemic health concerns in research studies.
The Link Between Gum Disease and General Health
Organizations such as Centers for Disease Control and Prevention and World Health Organization have discussed associations between periodontal disease and systemic conditions in certain populations.
However, these associations do not mean every person with periodontitis will develop broader health complications.
Why Early Evaluation Matters
Early diagnosis allows dental professionals to identify disease stage, evaluate risk factors, and recommend appropriate monitoring before additional structural changes occur.
Periodontitis in Dogs: A Separate Condition
Some searches for “periodontitis” relate to pets rather than humans. Gum disease in dogs follows different patterns and requires veterinary care instead of human dental treatment methods.
Canine Gum Disease Has Different Signs
In dogs, signs may include:
- Difficulty eating
- Excessive drooling
- Visible tartar buildup
- Bad breath
Human periodontal staging systems do not apply to animals.
Why Veterinary Evaluation Is Important
Only a veterinarian can properly evaluate canine oral health and recommend suitable treatment or imaging for pets.
Take the Next Step for Your Gum Health at AllSmiles Dental Care
Periodontitis is a progressive condition, but catching it early makes a significant difference. Whether you are noticing occasional bleeding gums or more persistent changes, getting a professional assessment is the most reliable way to understand what stage you may be at and what steps to take next. The sooner it is identified, the more options are available to slow or manage its progression effectively.
If you are concerned about your gum health, the team at AllSmiles Dental Care can help you get a clear picture of where things stand and guide you through the right care plan for your situation. Book consultation now, here!
FAQ About Periodontitis Disease
Is periodontitis serious?
Yes, periodontitis can become serious if untreated because it may damage the tissues and bone supporting the teeth.
Can periodontitis go away on its own?
It usually does not resolve on its own once deeper supporting tissues are affected. A dental evaluation is important to understand what stage it may be at and what monitoring or treatment is appropriate.
Can periodontitis kill you?
Periodontitis itself is not typically described in those terms, but severe untreated gum disease has been linked with broader health concerns in research from organizations such as the CDC and WHO. If you have concerns, a dental or medical review can help clarify the situation.
